22-24 However, the difference declines as patients get older. 21Ĭonsidering gender, short term (in-hospital/30-day) mortality and long term mortality after myocardial infarction is higher in women compared to men this is observed in younger women less than 55 years old. Studies have found that patients admitted to hospitals with a low volume of MI patients had a higher risk of mortality, as compared to patients admitted to hospitals with high MI patient volume (hazard ratio = 1.17 95% CI 1.09-1.26). 20 Hospital experience is also a factor in survival of myocardial infarction patients. 19 Myocardial infarction patients cared for by a cardiologist have lower mortality than those cared for by other clinicians. 19-20 Patient survival is significantly increased if the clinician handles more than 24 MI cases per year (19.6% patient mortality per year), as compared to clinicians who handle less than 5 MI patients per year (24.2% patient mortality per year). The experience of the clinician managing the patient with MI affects patient survival. 16-18 Also, these patients tend to have more comorbidities such as hypertension, diabetes, and stroke. Bundle branch block progresses to second or third degree AV block. The risk of mortality is increased in these patients. Left bundle branch block (LBBB) and right bundle branch block (RBBB) often precede MI. The risk of death in these patients is lower than those with a culprit lesion. These may be due to rapid clot lysis, vasospasm, or coronary microvascular disease. 10-11 Collectively, they are known as MI with normal coronary arteries.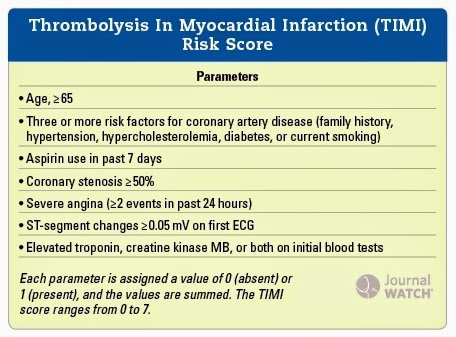  
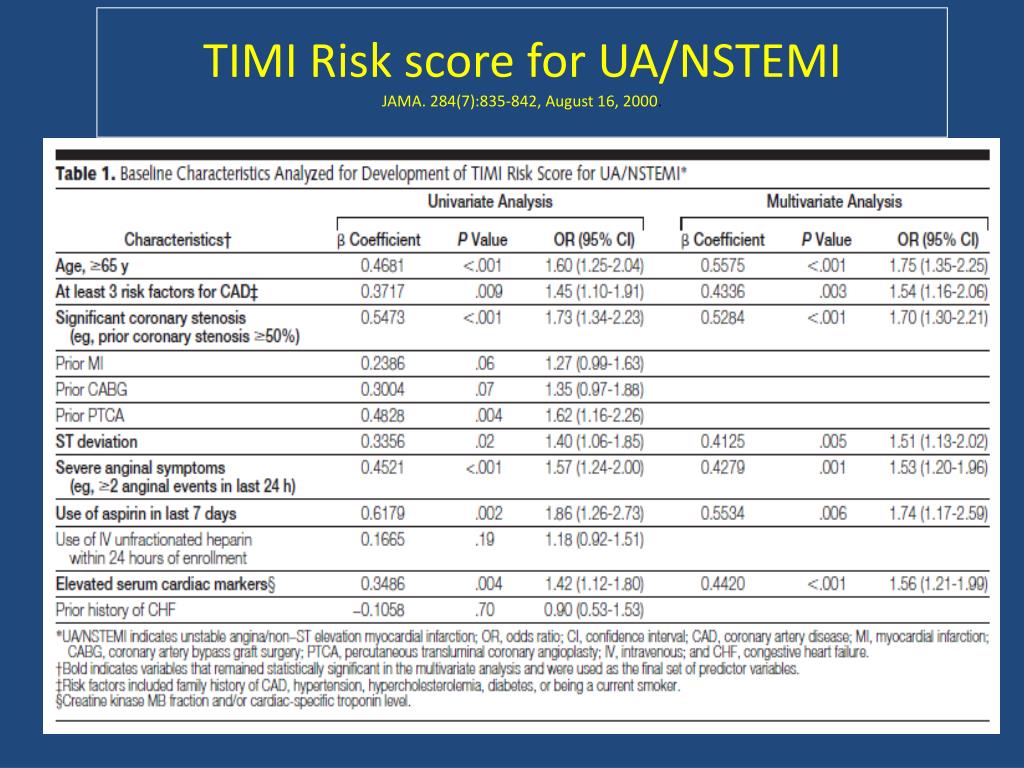
Normal coronary arteries or no vessel with ≥50% stenosis is observed in 12% to 14% of patients with NSTEMI and 7.5% of patients with STEMI. They have an increased risk for complications and death, especially if the location of the next infarct is far from the previous cardiac event. 14Īs mentioned earlier, patients with a history of myocardial infarctions are likely to have a recurrent MI. The risk of death is more pronounced in patients with moderate to severe mitral regurgitation compared to mild mitral regurgitation. TIMI risk scores: 0-1 points (3% to 5%) 2 points (3% to 8%) 3 points (5% to 13%) 4 points (7% to 20%) 5 points (12 % to 26%) 6-7 points (19% to 41%).Ī common complication of myocardial infarction is ischemic mitral regurgitation, which is due to infarction with annulus dilatation or displacement of the papillary muscle secondary to changes within the left ventricular anatomy following a cardiovascular event. ST deviation greater than 0.5mm (1 point).Severe angina in the preceding 24 hours (1 point).Aspirin use in the past 7 days (1 point).Known CAD with more than 50% stenosis (1 point).Thrombolysis in Myocardial Infarction (TIMI) score for unstable angina or non ST elevation myocardial infarction (NSTEMI). 12-13 The higher the score, the more the patient is at risk of mortality from cardiac events (Table 1 and Table 2). The most commonly used scoring system is the TIMI risk scores for STEMI and NSTEMI. Risk scores gauge the outcome after an acute MI. The risk of death after a myocardial infarction is determined by understanding the predictors of mortality. 10-11 The utilization of early invasive reperfusion techniques in NSTEMI patients will likewise decrease MI recurrence, rehospitalization and mortality. 6-9 There is an even lower risk of death of only 2% in patients with non-ST elevation myocardial infarction ( NSTEMI) after 30 days, as compared to STEMI. 5 Thirty day mortality rates are 13% with medical therapy alone, 6-7% with optimal fibrinolytic therapy, and 3% to 5% with primary percutaneous coronary intervention when performed within 2 hours of hospital arrival. In ST-elevation myocardial infarction ( STEMI), the increased use of fibrinolytic therapy and primary percutaneous intervention (aka angioplasty with stent), in conjunction with the increased use of aspirin, ACE inhibitors, statins and beta-blockers, has improved mortality rates. 1 The goal of reperfusion interventions is to limit the amount of permanent myocardial damage, necrosis, and scar tissue formation. However, due to recent developments in reperfusion techniques, in-hospital death rates have decreased from 5.3% to 3.8%. During the first 30 days after a myocardial infarction, death can occur due to cardiogenic shock, sudden cardiac death, heart failure, mechanical cardiac complications, or another MI event. A person who has experienced myocardial infarction (MI) is likely to experience other cardiovascular events.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
